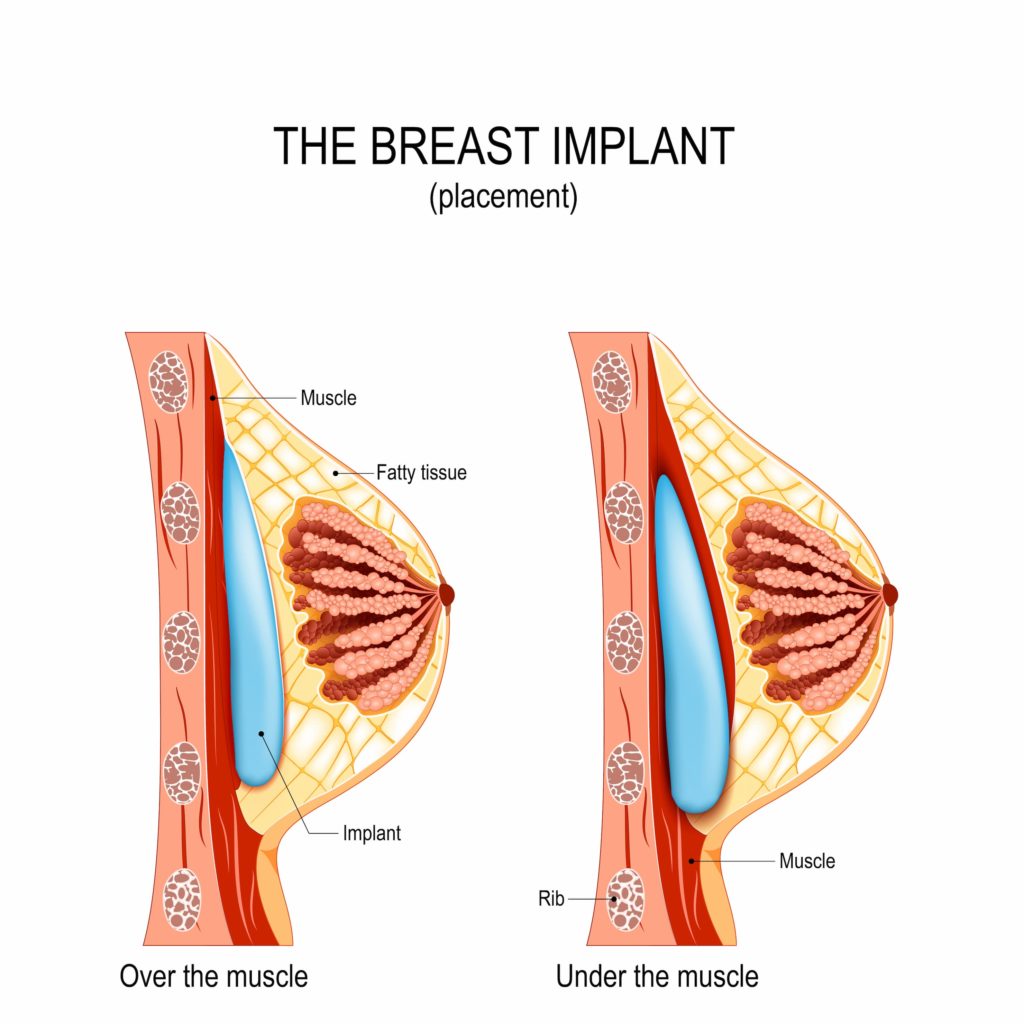
For more than a decade, I have been refining my technique for breast augmentation. During that time, I have also been unique in my preference of sub-glandular implant placement. I was trained to perform the procedure by placing the implants under the muscle, but I have looked past that habit with a challenging and practical perspective.
It has always occurred to me that the breast actually belongs and lives over the pectoralis muscle. Implant placement in the space beneath it is a continual tug-of-war between the foreign body, the rib cage, and what is left of the traumatized muscle. The old teaching was that only an Olympic athlete would notice a change in their function with the muscle lifted over a breast implant. Well, if that is true, then I must have a lot of secret Olympians in my practice; because nearly every time I meet a patient with sub-pectoral implants they mention that they have some limitation in function.
When patients come to me for a breast implant exchange, we go through all of the routine questions. We discuss implant size and position, type of fill, and their general lifestyle. If there is anything they would want to change about their augmentation, now is the time to do it. When I ask them if they want to keep the implant in the same plane, the conversation stops. It never occurred to them that they had the choice to do something different.
For many patients with sub-pectoral implants, especially if they have been in for a long time, they have gotten used to the functionality of the procedure, whether their limitation is small or significant. But once the pocket change is performed, the difference can be immediately appreciated. The implant is no longer being pulled up or fought with, and the implant-related pectoral animation deformities (look this up!) go away. The end result is often a better upper pole and a more functional upper torso.
A pocket change can also be very helpful if there are any significant implant positioning problems. Making a fresh pocket offers the surgeon an opportunity to sort of start from scratch. It can also help in cases where the patient has a significant capsular contracture or had a prior infection, by putting the new implant in contact with fresh tissue. All in all, there are many ways in which a pocket change resets the clock, or resolves a problem with the augmentation. It is not always the answer, but it should be considered as a possible option during an exchange.
During my career, I have heard every argument against sub-glandular augmentation. I disagree with these statements, as newer technology has produced far better devices, and surgical techniques are more refined. But most importantly, my many years of performing this procedure have shown me the extreme benefits to this approach, which honors natural anatomy and limits postoperative pain and problems. And as long as I keep hearing patients say “Wow, I never even knew it was an option to have the implants placed above the muscle. This feels so much better!” I will celebrate this approach, and use it strategically to heal others. Often, change is good.